People with ML III can live into adult life, as one of the more recently identified diseases it may be that there are even older adults living who have never been given the diagnosis of ML III.
Appearance
Onset of ML III is around 3 years old and is characterised by slow growth rate, the average height for adults with ML III is likely to be between 120cm to 165cm.
For some people the facial appearance may change little by the disease, while others may be affected in the same way as those with ML II. In situations where children are affected the neck is short, cheeks are often rosy and the nose may be broad with a flattened bridge and upturned nostrils. The mouth may be wide and overgrowth of the gums. Eyebrows may be bushy and meet in the middle and the eye sockets are shallow which makes the eyes appear prominent. People with ML III tend to have thickened and tough skin which lacks elasticity and occasionally there may be more body hair than normal, this is called hirsutism.
Brain
Many people with ML III will have no intellectual disabilities but some may have a learning disability which is often mild to moderate.
Heart
The heart may be affected in different ways. The muscles of the heart can be damaged by accumulation of unwanted molecules, this is called cardiomyopathy. The heart muscles are under strain by having to pump blood through stiffened lungs. The heart valves can be weakened and can fail to close tightly enough allowing small amounts of blood to leak back again. Problems with the valves can lead to valvular heart disease and if the condition worsens an operation may be needed to replace the damaged valves. An electrocardiogram (ECG) test is used to identify problems with heart muscle, function and valves, it is a painless procedure and is often carried out annually (or as often as the doctor thinks necessary) to show whether any problems are starting.
Lungs
Children with ML III are prone to frequent chest and ear infections and tend to have runny noses. In ML III the shape of the chest is affected and cannot move freely to allow the lungs to take in a large volume of air. Additionally, the tissue of the lungs becomes thickened by accumulation of unwanted molecules. This leads to an increase in secretions which are harder to clear as the restricted lungs make it difficult to take a deep enough breath to cough properly. When the lungs are not fully cleared there is an increased risk of infection which can lead to scarring causing further obstruction.
Medication for controlling cough and cold symptoms and mucus production is available but it is essential to consult the doctor rather than using ‘over the counter’ medication which may not help. Medications such as antihistamines may dry out the mucus making it thicker and harder to dislodge. Decongestants usually contain stimulants that can raise blood pressure and narrow blood vessels, both are undesirable effects for people with ML III. Cough medicines that have a sedating effect may cause more problems with sleep apnoea by depressing muscle tone and respiration. It is common for people with ML III to develop secondary bacterial infections which should be treated with antibiotics.
Liver, Spleen and Abdomen
The liver and spleen are not usually enlarged in people with ML III. The abdomen, due to weakness of the muscles of the tummy (abdominal) muscles, can lead to a hernia. A hernia is when an organ, such as the intestine, pushes through a weak spot in the muscle that holds it in place. Treatment options differ depending on the type of hernia, in some cases surgery is needed.
Bones and joints
Sometimes parts of the spine bones (vertebrae) in the neck do not develop properly but this is very unlikely to cause problems. X-rays or MRI scans can be used to diagnose or detect any problems that are present or likely to develop, and treatments usually involve spinal surgery or neck stability. There is a wide variation in the severity of problems. Skeletal problems may develop later in life. Some people may have stiff hips because the supporting socket is not formed properly. They may also have pain in their joints if they are very active. Surgery on the hips may be used as a last resort if pain becomes a real problem. Pain may also be relieved by warmth and the prescribing of analgesics. The limited movement in the shoulders and arms can make dressing difficult.
Hands
The shape of the hands is very noticeable, they are short and broad with stubby fingers which gradually become curved over or clawed. People with ML III sometimes experience pain, weakness or loss of feeling in the fingertips, this is caused by thickening of the ligaments which causes pressure on the nerves. It is called carpal tunnel syndrome and can be relieved by an operation. An electrical test called a nerve conduction study can show whether carpal tunnel syndrome is the cause.
Ears
Some degree of deafness is common in people with ML III. It may be conductive deafness, nerve deafness or both (called mixed deafness) and can be made worse by frequent ear infections.
Conductive deafness is when sound waves that travel through the ear canal, drum and the middle ear are impaired. Correct functioning of the middle ear depends on the pressure behind the ear drum being the same as that in the outer ear canal and the atmosphere. This pressure is kept equal by the eustachian tube which runs from the middle ear to the back of the nose. If the eustachian tube is blocked the pressure behind the eardrum will drop and the transmission of sound waves will be impaired. If this persists, fluid from the lining of the middle ear will build up and in time will become thick like glue, hence the condition being known as glue ear. Glue ear can be treated through surgery by inserting a small ventilation tube called a grommet, however these can fall out quickly and T-tubes, a type of grommet which stays in place longer, are an alternative option.
Nerve deafness is damage to the tiny hair cells in the inner ear. It may happen at the same time as conductive deafness, in which case it is referred to as mixed deafness. Mixed deafness can be managed by grommets or hearing aids. Nerve deafness is managed by fitting hearing aids in most people. More severely affected children may keep pulling out their hearing aids at first, but it is important to persevere at wearing them so that communication can be maintained. Alternatives include radio aids and the loop system which can be helpful at school and at home.
Eyes
People with ML III may experience clouding of the cornea which is caused by the accumulation of unwanted molecules, however this rarely interferes with vision and is not particularly noticeable.
Dental
Good dental hygiene is very important for children with ML III, teeth should be well cared for to avoid tooth decay, pain and extractions. Usually teeth are widely spaced and poorly formed with fragile enamel. Cleaning around the mouth with a small sponge or a stick soaked in mouthwash will help keep the mouth fresh and avoid bad breath. If the water in your area has not been treated with fluoride, speak with your dentist about including fluoride tablets or drops as part of the dental management plan. Dribbling is a common problem and can soak through clothes causing soreness, to prevent this choosing a bib that is plastic backed.
Where a child with ML III is severely affected it may be safer for any treatment to be carried out in hospital. If teeth need to be removed under anaesthetic this should be carried out in hospital under the care of an experienced anaesthetist and never in the dental surgery. It is important to inform the dentist about heart problems when discussing any treatment. This is because certain bacteria in the mouth may get into the blood stream and cause an infection on the heart valves. In most cases antibiotics are usually prescribed before and after any dental treatment.
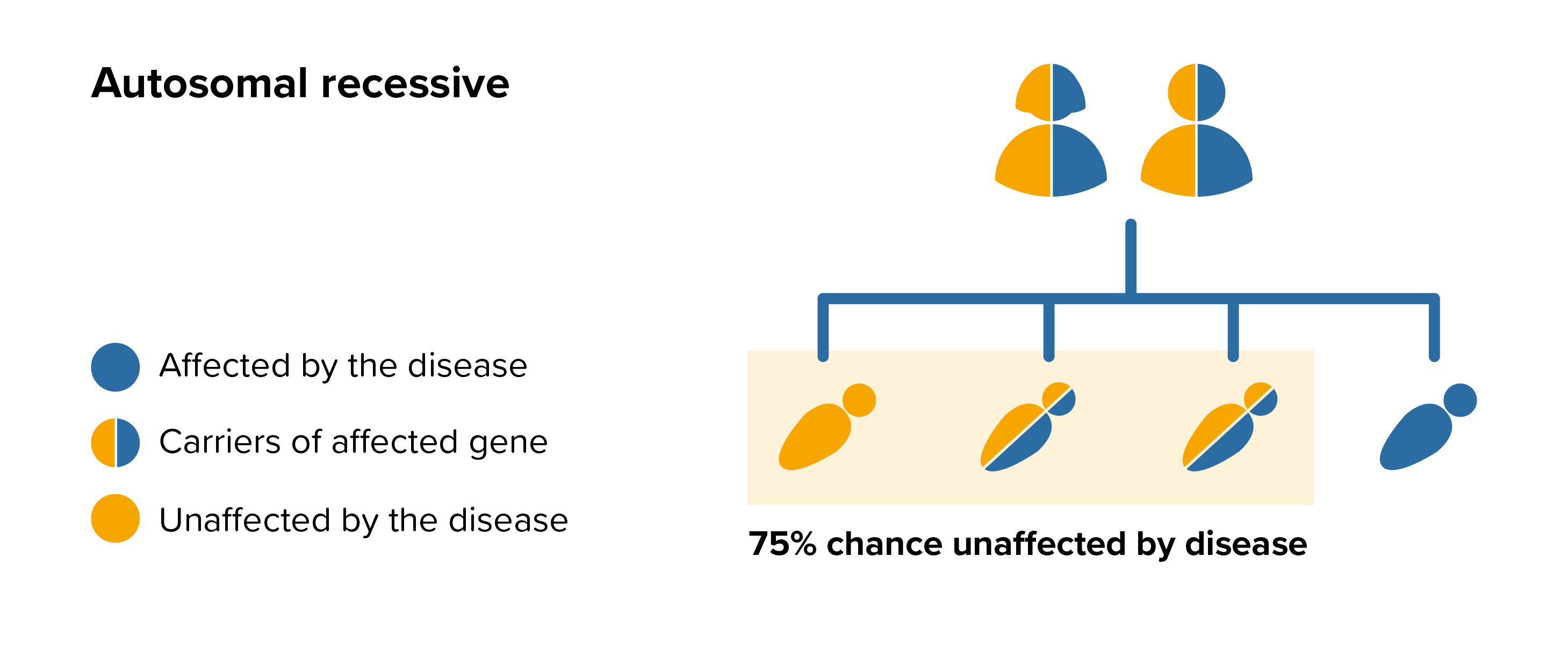 All parents of children with ML III can benefit from genetic counselling, the counsellor can provide advice on the risk to close relatives and to suggest whether the wider family should be informed. To find out during a pregnancy, if the baby is affected by ML III, screening tests can be arranged early on during a pregnancy for those families who already have a child with ML III. Where only one parent is a carrier, they can opt for carrier screening but it is not 100% reliable or accurate and is not possible in all cases.
All parents of children with ML III can benefit from genetic counselling, the counsellor can provide advice on the risk to close relatives and to suggest whether the wider family should be informed. To find out during a pregnancy, if the baby is affected by ML III, screening tests can be arranged early on during a pregnancy for those families who already have a child with ML III. Where only one parent is a carrier, they can opt for carrier screening but it is not 100% reliable or accurate and is not possible in all cases.



